|
| |
Issue no. 46 - September 1991
pdf
 version of this
Issue version of this
Issue
|
There is much information in this issue that is valuable
and useful. Online readers are reminded, however, that treatment guidelines and health
care practices change over time. If you are in doubt, please refer to
WHO's up-to-date Dehydration Treatment
Plans.
|
Pages 1-8 Dialogue on Diarrhoea Online Issue 46 -
September 1991
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  Page 1 2
Page 1 2
Best beginning: breastmilk
 |
The supportive atmosphere of group discussions helps give new mothers the confidence
to carry on breastfeeding.
|
Parents naturally want to give children a good start to make sure they grow up healthy
and do well, however poor their circumstances. Family feeding is highly important,
beginning with breastmilk for the newborn. But pressures on new mothers not to feed their
babies themselves are increasing. In this issue, we look at ways to help women feel more
confident about breastfeeding. Successful breastfeeding should be seen as the responsibility of the community at all
levels - local, national and international. In association with UNICEF, WHO, SIDA (the
Swedish International Development Agency) and USAID (the US Agency for International
Development), the Innocenti Declaration was signed in August 1990 by at least 30 national
representatives from around the world, promising to protect, promote and support
breastfeeding in their countries. Flexible approaches are required to meet the needs of
social change; the picture above shows urban mothers in the Philippines sharing their
experiences. When the baby is four to six months old, other foods must be gradually
introduced. Continued breastfeeding nevertheless helps to protect against infection
as well as providing valuable protein. Ideally breastfeeding should continue until the
child is accepting adequate amounts of suitable family foods. Commercial 'follow-up' milk
feeds are increasingly being promoted for these older infants, as a complement to
breastmilk. On="#page4">page 4 the problems and dangers of follow-up formulas
are discussed. There are also guidelines and an article on pages="#page6">6 and 7 on the health contribution gardens make to the family diet. Even with
limited resources, people can themselves do much to feed their families wisely.
|
In this issue:
- Support groups for breastfeeding mothers
- Update on the dangers of artificial milk feeds
- Guidelines on growing food for family health
|
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  1 Page 2 3 1 Page 2 3
Help for breastfeeding mothers
Talking and spending time in a small group with other mothers helps women to feel
confident about breastfeeding. DD reports on the activities of breastfeeding
support groups from around the world. Most women know that breastfeeding is the natural and best way to feed a baby.
Traditionally, young mothers learnt how to breastfeed from more experienced women in their
extended family and community. Nowadays, though, young women often have left their home
town or village and are isolated from women with whom they feel relaxed enough to learn
breastfeeding skills. Families, friends and even poorly informed health workers or doctors may feel that
bottle-feeding is as good as breastfeeding a baby. Artificial baby milks, or formulas, are
promoted internationally, but the dangers of bottle-feeding are not so well advertised
(see article on="#page4">page 4). Once a mother starts giving a bottle instead
of the breast, her breastmilk supply diminishes (which may lead to breastfeeding failure)
and it is difficult to re-establish breastfeeding. More women now give birth in hospitals, particularly in urban areas, where nurses are
busy or may not be trained in breastfeeding counselling. After she returns home, the
mother is often alone and has no support. Helping mothers
Most breastfeeding difficulties are not physical or medical. Of course, there are
exceptions: a mother who is seriously ill, or has a small, sick baby or a handicapped
infant, may need regular one-to-one support from a trained counsellor or health worker.
But problems usually arise because women have not been shown how to breastfeed properly,
fear that their breastmilk supply is inadequate, lack confidence in their skill, or feel
unable to combine breastfeeding with other responsibilities. One of the best ways to build up breastfeeding confidence in new mothers is to set up
support group meetings, where they can talk freely about their worries. These are some of
the common concerns:
- Emotional problems
Women need to feel sure they are providing enough of the best food for their babies.
Isolated and lonely young women are likely to stop breastfeeding if they are not finding
it straightforward, or worry that their babies are not thriving. A sympathetic partner,
doctor or health worker can provide important personal support, but the best help usually
comes from other mothers who know about breastfeeding.
- Social pressures
Breastfeeding can sometimes be difficult, particularly in an urban society. Mothers who go
out to work have to learn how to express and store their milk, and how to combine this
with continued breastfeeding. Some women may feel self-conscious and need to find the
confidence to breastfeed in public places. There may be pressure to follow harmful
practices, such as stopping breastfeeding when an infant has diarrhoea.
Support groups are very important in the Philippines. Poor women in urban
communities have to go out to work soon after they have given birth, and are under
pressure to start bottle-feeding. We visit new mothers in their homes to give them the
confidence to meet other women in a group.
A breastfeeding promotion logo used by the Breastfeeding Mothers
Support Group in Singapore.
At meetings we show women how to breasfeed, and use large and colourful pictures so that
they can see how their bodies work. We help women who want to express their milk, and also
explain how a child can be 'wet-nursed' by a breastfeeding friend when the mother is
working.
|
|
Ines Fernandez, ARUGAAN, The Philippines Practical difficulties New mothers will feel better and be healthier if they can get enough good food, and
gentle exercise only. The supportive atmosphere of a group will help give them confidence
to explain their needs to their families. How support groups work Mothers, with their babies, meet at least once a month, often in one of their own
homes. A few experienced breastfeeders need to be trained to act as group leaders. The leader introduces the subject, and then encourages the other women to join in.
She needs to be able to correct wrong information, and to put forward solutions to
problems. Topics include: advantages of breastfeeding; avoiding breastfeeding problems;
care of the newborn baby; and nutrition and weaning. Mothers also put forward their own
suggestions. Lorna McDougall, Breast is Best League, Belize Meetings are a way to learn:
- how to breastfeed easily and comfortably; for example, how to get the baby's suckling
position right;
- useful practical ideas about how to breastfeed at night, how to express and store
breastmilk, and how to breastfeed modestly in a public place;
- more information about how a woman's body works, and about children's growth and
development.
- Mothers also help each other outside meetings, and can advise women who are not regular
group members.
We give talks at youth groups, health centres and ante-natal classes. Our quarterly
newsletter is sent free to hospitals, clinics and doctors throughout Trinidad, Tobago and
Barbados. The telephone is one of our best methods of communication - a friendly
understanding voice is almost as good as seeing someone in person. Patricia Inglefield, TIBS, Trinidad and Tobago
|
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  2 Page 3 4 2 Page 3 4
How to set up a support group
- The best person to set up a group is a woman confident in social situations, experienced
in breastfeeding, and interested in learning leadership skills. Think about who could do
this in your community. Although willing to help lead a group, they may need assistance to
recruit members and set up and organise meetings.
- Start with one group. After a few months of successful meetings, some of the members
themselves will gain enough confidence to want training to set up and lead other groups.
- Find out how to get in touch with new mothers in your area. Tell health workers and
doctors about the group, and advertise at health centres where women take their babies for
check-ups. Staff at your local maternity hospital may be willing to recommend meetings.
Make sure local women's organisations, union branches or associations know about the
group, so that they can tell their members.
Some health workers used to feel that they were competing with support groups. Now
they understand that breastfeeding women need both caring, skilled health workers, and
caring, skilled friends. Health workers help us in publicising and setting groups up. One
support group in a rural area was called 'The Club', because at the time no one would come
to a group that had the word 'breastfeeding ' in its title! Having a thriving support
group (Nursing Mothers Association, Australia) in the town has made all the difference. Maureen Minchin, ALCA, Australia
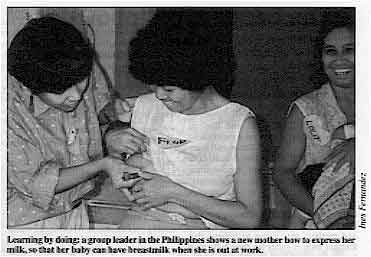 |
Learning by doing: a group leader in the Philippines shows a
new mother bow to express her milk, so that her baby can have breastmilk when she is out
at work. Contact your national breastfeeding promotion organisation. It can give advice about
setting up a support group, provide booklets and leaflets, and help with training group
leaders.
|
If there is no national group, then contact one of the="#International">international
organisations listed at the end of the article. I have been helping to run this support group network for many years. The two key
aims are to inform and inspire mothers about breastfeeding. Our organisation now has 50
members - all the members are trained group leaders, and most are fulltime mothers with
heavy family commitments. They run small support groups and give regular talks to
expectant parents at community centres, hospitals and clinics. We also keep a small
collection of useful books and articles, and produce a regular newsletter for our members.
The group has organised workshops for nursing staff at the maternity hospital, and is
helping them to put a breastfeeding policy into practice. Doris Fok, Breastfeeding Mothers Support Group, Singapore.
Some advantages of breastfeeding
Best for baby
Reduces incidence of allergies
Economical - no waste
Antibodies - greater immunity to infections
Stool inoffensive - never constipated
Temperature always correct and constant
Fresh milk - never goes sour in the breast
Emotionally bonding
Easy once established
Digested easily within two to three hours
Immediately available
Nutritionally balanced
Gastroenteritis greatly reduced
From a publicity leaflet by the TIBS support group, Trinidad.
DD
thanks all who contributed material on which this article is
based, including:
- Ines Fernandez, ARUGAAN (Support System for Working Women), 42 Maalalahanin St, Teachers
Village, Diliman, Quezon City, The Philippines
- Doris Fok, c/o Family Life Society, 257 Selegie Road, #02-273 Selegie Complex, Singapore
0718
- Patricia Inglefield, TIBS (The Informative Breastfeeding Service), 13 Rust St, Port of
Spain, Trinidad
- Lorna McDougall, Breast is Best League, 18 Eve Street, PO Box 1203, Belize City, Belize,
Central America
- Maureen Minchin, Australian Lactation Consultants' Association, c/o St George's Road,
Armadale, Victoria 3143, Australia
International breastfeeding support organisations
- Geneva Infant Feeding Association, P O Box 157, CH-1211 Geneva 19, Switzerland
- IBFAN Africa, P O Box 34308, Nairobi, Kenya
- ILCA, 201 Brown Ave, Evanston, IL 60202, USA
- Lactation Resource Centre, P O Box 231, Nunawading, Vic. 3131, Australia
- La Leche League International, 9616 Minneapolis Ave, Franklin Park, IL 60131, USA
The DD Health Basics="su37.htm">supplement on breastfeeding, together with
an updated list of resources and organisations, is available free of charge to readers.
| Feeding low birth weight babies, an IBFAN training video, is available in French,
Spanish and English versions from: Radio, Film and Television Section, Division of
Information. UNICEF, 3 UN Plaza, New York, NY 10017, USA (not from UNICEF Kenya as
reported in="dd41.htm">DD41). |
|
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  3 Page 4 5 3 Page 4 5
| Bottle-feeding and diarrhoea |
The dangers of 'follow-up' feeds
Ted Greiner explains why more action is needed to stop
the spread of bottle-feeding. Artificial feeds, or formula milks, made up with contaminated water, and unclean
feeding bottles and teats, are a major cause of diarrhoea in babies (1).
These milks are marketed internationally in two main categories: 'infant formula', sold as
a substitute for breastmilk, and 'follow-up formula' (sometimes known as follow-on
formula), sold as a complement to breastmilk for older infants.
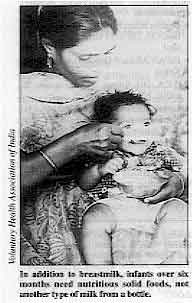 |
In addition to breastmilk, infants over six months need
nutritious solid foods, not another type of milk from a bottle. Manufacturers sometimes promote these products very aggressively, and mothers may come
to believe that formula milk is better for their baby than breastmilk. But breast is best
for all infants, and breastfed babies do not need either type of formula milk.
Follow-up formula need not be given to any infant even if s/he is over six months old -
older infants need solid nutritious foods combined with breastmilk.
|
What are the problems of follow-up formulas?
- Follow-up formula carries the same risk of infection as infant formula if bottles or
water are contaminated.
- Giving follow-up formulas can interfere with the weaning process, when the infant is
starting to eat family foods. Giving another type of milk, such as follow-up formula, as
well as breastmilk to an infant who is being weaned is expensive and may result in
replacing breastmilk, rather than complementing it, especially if given by bottle. The
1986 WHO World Health Assembly (in Resolution WHA39.28) stated that 'the practice being
introduced in some countries of providing infants with specially formulated milks
(so-called follow-up milks) is not necessary'. Nearly all countries voted in favour of
this resolution.
- WHO is also concerned that mothers could use follow-up formula by mistake instead of
infant formula (2). If follow-up formula is given to infants below six
months of age, its higher protein and mineral content increases the risk of dehydration
during diarrhoea
- These formulas can lead to an unbalanced diet. One study measured nutrient intakes of
infants at six to ten months of age likely to result from the use of two standard
follow-up formulas. With one, the infants received too much protein and with the other not
enough fat (3).
Why are companies promoting follow-up feeds?
The International Code of Marketing of Breastmilk Substitutes was drafted in 1981 by
WHO and UNICEF to reduce the spread of bottle-feeding. Many countries adopted a version of
this Code and have succeeded in regulating the marketing of some products. However, the
Code only controls how companies promote infant formulas which are known officially as breastmilk
substitutes (BMS): 'any food being marketed or otherwise represented as a partial or
total replacement for breastmilk, whether or not it is suitable for that purpose. ' In contrast, the Code does not cover follow-up formulas marketed as a complement to
breastmilk. Companies are now strongly promoting these in many industrialised and
developing countries and most families are not aware of the risks. A study done in Cebu
City in the Philippines shows how, in 1986, over half the health centres in the study gave
away free samples of infant formula, while only 15 per cent gave the mothers follow-up
formula samples (4). At the end of the year a code restricting the
promotion of infant formula was made law. Within two years the number of centres
distributing infant formula had decreased to under three per cent, but those giving away
free samples of follow-up formula had increased to 28 per cent. What action should be taken?
The increased promotion and use of follow-up formulas is putting breastfeeding and safe
weaning at risk. In some countries it may be possible to restrict the import or sales of
follow-up formulas altogether. In others you can ask your government to:
- Design and make law a national code which defines 'breastmilk substitutes' as any
product perceived and used as an alternative to breastmilk for young infants, even if
marketed as a breastmilk complement.
- If your country already has a national code, follow-up formulas can be added to the
definition of 'breastmilk substitutes' via, for example, a government order.
WHO will provide technical assistance on request to the government of any member
country on how to design, implement and monitor a national code. Ted Greiner, Department of Paediatrics, International Child Health Unit, Uppsala
University, S-751 85 Uppsala, Sweden.
1. Popkin, B M et al., 1990. Breastfeeding and diarrhoeal
morbidity. J. Ped. 86: 874-887.
2. World Health Organization, 1988. Observations on the proposed
draft standard for follow-up foods for older infants and young children. EB81/1988/ REC1,
Annex 10.
3. Fomon, S J et al., 1990. Formulas for older infants. J. Ped.
116:690-696.
4. Popkin, B M, 1990. Infant formula promotion and the health
sector in the Philippines. Amer. J. Public Health 80: 74-75. International Organization of Consumers Unions, 1989. Protecting infant health: a
health worker's guide to the international code of marketing BMS. This book, and
further information, is available from IOCU (IBFAN). P O Box 1945, 10830
Penang, Malaysia.
|
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  4 Page 5 6 4 Page 5 6
Reducing infection
Many studies in developing countries have demonstrated the importance of exclusive
breastfeeding until at least four to six months of age. A case control study in Brazil has
shown that young infants (0-2 months) who are not breastfed are 25 times more likely to
die as a result of diarrhoea than those who are exclusively breastfed (1). Even malnourished women can maintain growth of infants up to four to six months of age
by exclusively breastfeeding and not introducing other foods or liquids (2).
However, it is important to make sure that mothers are adequately nourished, to prevent
their losing too much weight while they are breastfeeding.
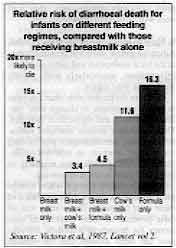 |
Relative risk of diarrhoeal death for infants on different
feeding regimes, compared with those receiving breastmilk alone Source: Victora et al, 1987, Lancet vol 2. Infants are more likely to get infections if they are given milk supplements by bottle.
In the Brazil study, the relative risk of dying from a diarrhoea infection was found to be
much higher for infants fed on formula or cow's milk than for those fed on breastmilk only
(see graph). Giving other supplements carries a similar risk.
|
A finding from a study in the slums of Lima, in Peru, was that infants less than five
months old given liquids apart from breastmilk, such as tea and water, were twice as
likely to get diarrhoea (3). Even in very hot climates, infants do not
need water in addition to breastmilk (4). Continued breastfeeding reduces the risk of infection during weaning. Infants aged six
months to one year who were receiving breastmilk along with weaning foods or other milk
had less diarrhoea than those whose diet did not include breastmilk (1),
(3). Hospital based studies in Pakistan, Costa Rica, India and the Philippines have shown
that where women were encouraged to breastfeed in hospital neonatal wards, where
bottle-feeding was the norm, rates of neonatal diarrhoea consistently decreased.
Breastfeeding also helps to prevent dehydration. In Myanmar a study compared stool output
of infants with diarrhoea who continued to be breastfed, as well as being given ORS, with
that of those given ORS alone. The breastfed infants passed fewer stools and therefore had
less dehydration (5). 1. Victora, C G, et al, 1987. Evidence for protection by
breastfeeding against infant deaths from infectious diseases in Brazil. Lancet: 2: 319-21.
2. Brown, K H et al,
1986. Lactational capacity of
marginally nourished mothers. J. of Ped; 78: 909-919.
3. Brown et al, 1988. Infant feeding practices and their
relationship with diarrhoeal and other diseases in Huascar (Lima), Peru. J.
Ped. 83:
31-44.
4. Almroth, S and Bidinger P 1990. No need for water
supplementation for exclusively breastfed infants under hot and arid conditions. Trans. R.
Sot. Trop. Med. Hyg. 84: 602-604.
5. Khin-Maung et al, 1985. Effect on clinical outcome of
breastfeeding during acute diarrhoea. Brit. Med. J. 290: 587-89. Abstract taken from: Huffman S and Combest C, 1990. Review article: Role of
breastfeeding in the prevention and treatment of diarrhoea, J. Diar. Dis. Res. 8:
68-81. If readers would like further references, please contact DD at
AHRTAG. Baby-friendly hospitals
UNICEF and WHO are helping to promote breastfeeding by suggesting that hospitals adopt
guidelines along the following 'ten steps':
- Develop a written breastfeeding policy and make sure that the staff support it.
- Train staff how to help new mothers to breastfeed successfully.
- Tell pregnant women about the benefits of breastfeeding.
- Help mothers to begin breastfeeding within half an hour of birth.
- Show mothers how to breastfeed, and how to continue giving breastmilk even if they are
away from their infants.
- Give newborn infants no food or drink other than breastmilk, unless medically indicated.
- Arrange for mothers and infants to stay in the same room together (rooming-in).
- Encourage breastfeeding on demand.
- Discourage giving artificial teats to breastfeeding infants.
- Recommend local breastfeeding support groups to new mothers.
Source: Protecting, promoting and supporting breastfeeding: the special role of
maternity services. WHO/UNICEF, 1989, Geneva. This approach was endorsed at the 1991
international paediatrics conference in Turkey. Dummies and diarrhoea
I have noticed that many people use pacifiers (or dummies) in this part of the world.
Does their use contribute to the spread of diarrhoea in infants? Dr Satya K Narayana, P O Box 176, Aligoudarz,
Lorestan, Iran. Dr Katherine Elliott comments on the increasingly widespread use of pacifiers.
Pacifiers (also called comforters or dummies) are artificial teats or nipples usually
made from rubber or plastic, which are given to small babies or children to suck. Sucking
is an instinctive action, not something we learn. Modem technology has shown us how we
even suck our thumbs within the womb before birth. Small babies like to suckle frequently,
using the nipple both for comfort and for food. So it is not surprising that pacifiers were developed to calm babies between feeds and
allow mothers some freedom. Their use would be comparatively harmless in ideal hygienic
conditions. But, just as with feeding bottles and their teats, problems arise where
environmental conditions are poor or if families do not realise the dangers of
contamination by contact with dirty hands, clothes or floors. A pacifier can easily carry
the bacteria which cause diarrhoea. Even if the mother is careful, older children often
pick up the pacifier and put it back in the baby's mouth, and toddlers who have become
addicted to sucking a pacifier will do it for themselves. Babies cry because they are hungry or unhappy in some way and their needs ought to be
understood and satisfied. Unusual circumstances may sometimes justify the occasional use
of a pacifier - for example, to get a really fretful baby to sleep in disturbed or
emergency conditions. We are all aware of the risks of bottle-feeding in relation to
diarrhoea. Pacifiers carry the same risks and their use is an unnecessary habit which
everyone should try to discourage.
|
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  5 Page 6 7 5 Page 6 7
Growing food: growing healthy
DD gives some practical guidelines for setting up gardens to improve family
diet. Home and community gardens are an important source of food. Vitamin-rich vegetables and
fruit added to the family diet can improve children's nutritional status and resistance to
infections. The following is a checklist of things for community workers or nutritionists to think
about before starting a garden project. 1. Talk to people about what is already happening.
Find out how many people already grow vegetables. Ask where the gardens are, who looks
after them and what vegetables and fruit are usually grown. Ask if these are sold, or if
some are eaten at home. Find out what people usually eat. Find out about available land
for new gardens, and what the soil type is. Gardens must be appropriate for the community,
and if people feel involved from the start, they will find it easier to change how they
garden and what they eat. 2. Find out about health problems.
Ask how many children have health problems such as vitamin deficiencies or
malnutrition. The success of the gardens can be measured by improved community health. 3. Start small.
Begin with a few households only, or with a garden at a school or health centre. If
families like the results, the new ideas will soon spread. Listen to local people about
traditional gardening methods, and involve them in the new project.
 |
Adding home grown fruit and vegetables to the family diet is an
inexpensive and convenient way to improve children's nutritional status. The drawing
shows, from left to right, 'green leaves' oranges, carrots, tomatoes, a guava and spinach.
|
4. Choose the right things to grow.
Promote only one or two vitamin-rich vegetables or fruits at the beginning,
particularly those already grown locally. Remember that different crops may grow during
different seasons, and methods of storage and preservation may need to be developed. Carrots and other root vegetables and small fruit trees such as banana, papaya, mango,
guava, breadfruit, citrus and coconut are all good value - as are tomatoes, pumpkins and
peppers. If they get enough water, many different kinds of dark green leafy vegetables are
easy to grow, and provide useful protein as well as vitamin A. Look for local varieties.
(See also those listed in the case study.) In some countries, wild plants are eaten
regularly and these can be a valuable source of vitamins. 5. What do gardens need?
- Water
A water supply is needed near the garden. Irrigation channels, terraces, rain and
run-off water storage, and drought resistant plants help save water in dry climates, but
in some countries and during rainy seasons, too much water has to be drained away.
Domestic waste water that is not contaminated with faecal waste can be used to water
plants. Raw fruit and vegetables must be properly washed before eating to avoid diarrhoea
infections.
- Protection
To keep animals out, use local fencing materials which are cheap and easy to replace.
If a fence is not practical, try to protect the plants themselves. For example, in
backyard gardens in the South West Pacific, coconut husks around plants stop domestic
chickens from eating the stems.
- Compost and pest control
Make organic composts from garden, household and animal waste, and control pests with
locally available materials, such as soap, tobacco, garlic and oil. Commercial fertilisers
and pesticides are expensive, and can be dangerous.
- Seeds
Local plant varieties are often the best, since their seeds can be stored each year for
the next season. Imported seeds are usually hybrid varieties which do not produce reliable
seeds. If you use plants new to the region, make sure you can provide seeds for the next
year. Set up a small nursery to grow seedlings for other people. Some vegetables, such as
potatoes and yams, grow from root cuttings and many fruit trees will grow from branch
cuttings.
6. How to make the project successful.
Advertise garden visits and demonstrations in the local newspaper and radio, and share
information, particularly with people working in your region. Combine the project with other activities to encourage people to change their gardening
methods and supplement their diet. These activities include nutrition education, cooking
demonstrations and training community workers in relevant skills. Measure child growth
rates regularly to find out if their health is improving. A project study in Senegal where women grew vegetables shows the importance of these
extra activities. The women sold all their produce in local markets to earn money for
household expenses. Surveys over ten years showed that the vitamin intake of their
children did not increase and that income from selling vegetables was almost never used
for buying food'. If most people sell what they grow, you may need to help them improve
their income by more effective marketing and so make it financially possible to keep aside
some vegetables for family meals. 1. Marek et al, 1990. Do home gardens improve income and
nutritional status? A case study in Senegal. Food and Nutrition Bulletin, 12, no I.
|
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  6 Page 7 8 6 Page 7 8
Case study: gardening in The Gambia
Home and school gardens are common in The Gambia. Most of the produce is sold in nearby
markets. However, during the drought in the 1970s many people stopped growing vegetables.
In 1985 the school and community gardening project was introduced. Gardens are made by fencing off a few acres of land with one or two irrigation wells.
These community plots are divided into beds of a few metres long by one metre wide. In the
schools involved in the programme, groups of children look after the plots, with the help
of the teacher. During practical teaching sessions, they learn about how eating the
vegetables they grow can make them healthier. The programme aims to:
- set up and look after school gardens;
- use school gardens to help children learn about nutrition;
- improve children's diets by increasing the amount of vegetables in school meals;
- grow enough produce for some to be sold to generate income;
- involve family members in looking after the gardens;
- encourage people to stay in rural areas, by showing that gardening and farming can
generate income, as well as improve nutrition.
Fruit / vegetable promoted by the project
|
Nutrient
|
| Carrot, cassava leaf, lettuce, local greens, sweet potato, tomato, water
melon, banana, cashew apple, mango, papaya |
Vitamin A |
| Banana, cashew apple, citrus, mango, papaya, guava, cabbage, lettuce,
okra, tomato, sorrel, pepper |
Vitamin C |
| Okra, garden egg (aubergine variety), bitter tomato, local greens |
Vitamin B |
| Local greens, cassava leaf, okra, sorrel, carrot, lettuce, 'never-die' |
Iron |
| All vegetables and fruits have varying degrees of mineral content |
Minerals |
Local and imported varieties of vitamin-rich fruit and vegetables are
grown. All these grow well during the dry season from October to March. Local varieties
(local greens, okra, pepper, bitter tomato, sorrel) are resistant to pests and diseases
that spread during the rainy season; these are grown throughout the year.
|
It is important to make the links between
growing vegetables and the benefits of a better diet. During practical teaching sessions
these Gambian school children learn about how eating the vegetables they grow can make
them healthier.
The schools encourage a low cost approach to gardening. People are advised to use
organic manure (animal waste and compost) instead of artificial fertiliser. Cheaper and
often safer alternatives to chemical pesticides are used for pest control. Household ash
can be sprinkled around plant stems, helping to protect the root from pests. A pesticide
can be made from boiling a handful of neem tree leaves, hot peppers and tobacco or a
handful of onion skins in a panful of water. The mixture is then strained and sprayed or
sprinkled onto the crop. 'Companion planting' - growing marigolds or garlic next to the
main crop - can help to keep certain pests under control.
|
 |
The project hopes to pass on information about nutrition to the community through:
- organising visits to the school garden;
- showing people how to garden more effectively;
- encouraging the children to talk about the garden at home or when working in the
community garden with their mothers.
This approach seems to be successful. There are now more community gardens in areas
where school projects have been set up. More people are including fruit and vegetables in
their diets, particularly in schools, where over half of the garden produce is eaten by
the children. In most communities children and women are looking healthier, and there are
fewer cases of malnutrition. Mbye Njie and Anne Plested (supported by Voluntary Service Overseas, UK), School
Farm and Garden Field Co-ordinators, Ministry of Education, The Gambia.
A full account of VSO's involvement in this programme will be included in the
forthcoming VSO publication 'Making Agricultural Education Relevant'. For more information
write to Programme Evaluation, VSO, 317 Putney Bridge Road, London SW15 2PN, UK. Resources
- Sommers P, 1984. Home gardens handbook for people promoting mixed gardening in the
humid tropics. Programme Publications, UNICEF, 3 UN Plaza, New York NY 10017, USA. $5
per copy.
- Cleveland D, and Soleri D, 1991. Food from dry land gardens. Center for People,
Food and Environment, 344 South Third Avenue, Tucson, AZ 85701, USA. $15 per copy ($ 25 to
workers and projects sponsored by Western aid agencies).
- Garden to kitchen newsletter from: Family Food Production and Nutrition Project,
UNICEF Pacific Operations, c/o UNDP, Private Mail Bag, Suva, Fiji.
- The following are available free from the Vitamin A Field Support Project (VITAL), 1601
N. Kent Street, Suite 1016, Arlington, VA 22209, USA:
- Soleri D, et al. 1991. Vitamin A nutrition and gardens bibliography.
- Peduzzi C, 1990. Home and community gardens assessment program implementation
experience: the tip of the iceberg.
- Soleri D, et al. 1991. Gardens and vitamin A: a review of recent literature.
|
|
DDOnline
Dialogue
on Diarrhoea Online Issue no. 46 September
1991  7 Page 8 7 Page 8
Collaborating on cholera
First seen in Latin America in Peru in January, cholera had spread to Ecuador,
Colombia, Brazil, Chile and Mexico by June 1991. Over 220,000 cases have been reported;
80,000 people have been admitted to hospital, and there have been 2,200 deaths. In April, a team of experts from the International Centre for Diarrhoeal Disease
Research in Bangladesh (ICDDR, B) went to Ecuador. Their visit gave Ecuadorean
public health workers and doctors the chance to discuss cholera control and management
with professionals from another developing country with a wealth of useful experience.
Cholera is endemic in Bangladesh, and the ICDDR, B hospital admits many cases of cholera a
day. The team's recommendations included: Epidemiology
- setting up systems to help local health personnel detect cholera;
- looking into suspected cholera deaths to find out why patients died;
- making sure that epidemiologists throughout the country are aware of surveillance
procedures.
Microbiology
- setting up more laboratories to identify cholera organisms;
- making sure the vibrio survive (using Cary-Blair media) during the journey to the
laboratories;
- using vibrio cultures to monitor epidemic spread (rather than to confirm the diagnosis
in clinically obvious cholera).
Case management
- writing guidelines on how to clinically assess and manage diarrhoea in patients;
- setting up temporary treatment centres where there are few health facilities;
- using cholera cots to check how much fluid the patient is losing;
- giving food to patients as well as ORT.
Governments in the region, together with WHO, PAHO and USAID are now developing a
co-ordinated plan of action to control cholera in Latin America. Source: Jim Trostle, Applied Diarrhoeal Diseases Research Project
(ADDR), HIID, I
Eliot St, Cambridge, Mass. 02138, USA. ADDR coordinated the team's visit to Ecuador:
Progress in ORT
The May 1991 issue of the popular and respected magazine Scientific American
features a comprehensive review by Norbert Hirschhorn and William B Greenough of all
aspects of ORT. Dr Norbert Hirschhom has been a member of the Dialogue's editorial
advisory board since the newsletter began in 1980.
Drugs and dysentery
I read the="su44.htm">supplement on shigellosis in DD44 with keen
interest. However, we have been taught in the laboratory to use nalidixic acid, along with
nitrofurantoin, on urinary pathogens only. Is treating shigellosis with nalidixic acid a
new development? Terrence Akaa Ijir, P 0 Box 491, Makurdi, Benue State, Nigeria.
Dr Bennish and Dr Salam (authors of the supplement) reply:
Nalidixic acid is used for treating acute dysentery only in areas where Shigella are
resistant to ampicillin and cotrimoxazole. But your letter raises an important point. You
are correct that nalidixic acid, like nitrofurantoin, has been used in the past only for
the treatment of urinary tract infections. This is because nalidixic acid given by mouth
is poorly absorbed, and the concentration of the drug is therefore too low to be effective
against most infections. The exception to this has been infections of the urinary system,
as nalidixic acid is excreted by the kidney and concentrated in the urine. We have shown that nalidixic acid is absorbed sufficiently to be effective in the
treatment of Shigella infections (1). We recommend routinely testing all
Shigella isolates for susceptibility to nalidixic acid, as well as the standard
antibiotics. If the prevalence of resistance to ampicillin and cotrimoxazole is more than
ten per cent, nalidixic acid is recommended. 1. Salam, M A and Bennish, M L, 1988. Therap) for shigellosis:
randomized, double blind trial of nalidixic acid in childhood shigellosis. J.
Ped. 133:
901-7.
Success in Trinidad
We have benefited a great deal from the information in
DD. The Health Basics="su19.htm">supplement on oral rehydration therapy helped us enormously in our
teaching sessions with parents, student nurses and other health personnel. We wish the
newsletter another successful decade! In our unit we are celebrating ten years of controlling diarrhoea by the use of oral
rehydration therapy. When we started the unit we encountered problems similar to those
experienced in other countries, especially in getting parents and doctors to accept this
type of treatment. We have overcome most of these problems successfully. Now nearly 60 per cent of our
children have appropriate home fluids at home before coming to the unit for follow-up
treatment. Our success is due to health education programmes carried out at the unit and
health centres, and in the mass media. Cynthia Scipio, ORT Unit, General Hospital, Port of Spain, Trinidad.
Ed: The Health Basics ORT supplement is still available to readers from
AHRTAG.
|

Scientific editors Dr Katherine Elliott and Dr William Cutting
Managing editor Kathy Attawell
Assistant editor Nel Druce
Editorial advisory group
Professor J Assi Adou (Ivory Coast)
Professor A G Billoo (Pakistan)
Professor David Candy (UK)
Professor Richard Feachem (UK)
Dr Shanti Ghosh (India)
Dr Michael Gracey (Australia)
Dr Nicole Guérin (France)
Dr Norbert Hirschhorn (USA)
Dr Sharon Huttly (UK)
Dr Claudio Lanata (Peru)
Professor Leonardo Mata (Costa Rica)
Dr Jon Rohde (USA)
Dr Mike Rowland (UK)
Ms E O Sullesta (Philippines)
Professor Andrew Tomkins (UK) With support from AID (USA), ODA (UK), UNICEF, WHO
Publishing partners
BRAC (Bangladesh)
CMAI (India)
CMU (China)
Grupo CID (USA)
HLMC (Nepal)
lmajics (Pakistan)
ORANA (Senegal)
RUHSA (India)
Consultants at University Eduardo Mondlane (Mozambique)
|
Issue no. 46 September 1991
Page Navigation
This edition of Dialogue on Diarrhoea Online is produced by Rehydration Project. Dialogue on Diarrhoea was published four times a year in English, Chinese, French, Portuguese, Spanish, Tamil,
English/Urdu and Vietnamese and reached more than a quarter of a million readers worldwide. The English edition of Dialogue on Diarrhoea was produced and distributed by Healthlink Worldwide. Healthlink Worldwide is committed to strengthening primary health care and
community-based rehabilitation in the South by maximising the use and impact
of information, providing training and resources, and actively supporting
the capacity building of partner organisations. - ISSN 0950-0235 Reproducing articles
Healthlink Worldwide encourages the reproduction of
articles in this newsletter for non-profit making and educational uses. Please
clearly credit Healthlink Worldwide as the source and, if possible, send us a copy of any uses made of the material.
|
updated: 23 August, 2019
|