ACUTE DIARRHOEA STILL A LEADING CAUSE OF CHILD DEATHS
|
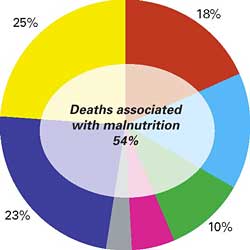 Major Causes of death among children Major Causes of death among children
under five in developing countries, 2002
|
Though the mortality rate for children under five suffering from acute diarrhoea
has fallen from 4.5 million deaths annually in 1979 to 1.6 million deaths in
2002, acute diarrhoea continues to exact a high toll on children in developing
countries.Oral rehydration salts (ORS) and oral rehydration therapy (ORT), adopted by
UNICEF and WHO in the late 1970s, have been successful in helping manage
diarrhoea among children. It is estimated that in the 1990s, more than 1 million
deaths related to diarrhoea may have been prevented each year, largely
attributable to the promotion and use of these therapies. Today, however, there
are indications that in some countries knowledge and use of appropriate home
therapies to successfully manage diarrhoea, including ORT, may be declining.
 Acute respiratory infections Acute respiratory infections
|
 HIV/AIDS HIV/AIDS |
 Diarrhoea Diarrhoea |
 Perinatal Perinatal |
 Malaria Malaria |
 Other Other |
 Measles Measles |
|
|
Sources: For cause-specific mortality: The World Health Report 2003, WHO, Geneva.
For malnutrition: Pelletier, D. L., E. A. Frongillo, and J. P. Habicht,
‘Epidemiologic evidence for a potentiating effect of malnutrition on child
mortality’, American Journal of Public Health, vol. 83, no. 8, August 1993, pp.
1130-1133. Note: The figures for proportional mortality related to children under five are
currently under review by UNICEF and WHO.
|
THE GOALS
The revised recommendations will help reduce mortality from diarrhoea, in line
with global goals that aim to:
- Reduce by one half deaths due to diarrhoea among children under five by 2010
compared to 2000 (‘A World Fit for Children’, outcome document of the UN Special
Session on Children)
- Reduce by two thirds the mortality rate among children under five by 2015
compared to 1990 (United Nations Millennium Development Goals)
JOINT STATEMENT
More than 1.5 million children under five continue to die each year as a result
of acute diarrhoea. The number can be dramatically reduced through critical
therapies such as prevention and treatment of dehydration with ORS and fluids
available in the home, breastfeeding, continued feeding, selective use of
antibiotics and zinc supplementation for 10–14 days.
These new recommendations, formulated by UNICEF and WHO in collaboration with
the United States Agency for International Development (USAID) and experts
worldwide, take into account new research findings while building on past
recommendations. Success in reducing death and illness due to diarrhoea depends
on acceptance of the scientific basis and benefits of these therapies by
governments and the medical community. It also depends on reinforcing family
knowledge of prevention and treatment of diarrhoea, and providing information
and support to underserved families.
PROGRESS AND CHALLENGES
NEW DEVELOPMENTS
Recent scientific advances have informed these revised recommendations. They
are:
- Development of an improved formula for ORS solution with reduced levels of
glucose and salt, which shortens the duration of diarrhoea and the need for
unscheduled intravenous fluids1
- Demonstration that zinc supplements given during an episode of acute diarrhoea
reduce the duration and severity of the episode2, and
- Findings that zinc supplementation given for 10–14days lowers the incidence of
diarrhoea in the following 2–3 months3
Many more lives can be saved if these advances are used in conjunction with
effective home treatment and use of appropriate health services. To be most
effective, these revised recommendations must become routine practice both in
the home and health
facility. (See the Technical Annex on page 6 for additional
details.)
BUILDING ON PAST SUCCESSES
 |
ORS, ORT and other components of clinical management of diarrhoea have made a
significant contribution to reducing deaths from diarrhoea. However, if the
global goals are to be met, there is still much to do.Family knowledge about diarrhoea must be reinforced in areas such as prevention,
nutrition, ORT/ORS use, zinc supplementation, and when and where to seek care.
Where feasible, families should be encouraged to have ORS ready-to-mix packages
and zinc (syrup or tablet), readily available for use, as needed. Breastfeeding
should continue simultaneously with the administration of appropriate fluids or
ORS. |
RECOMMENDATIONS
The revised recommendations emphasize family and community understanding of
managing diarrhoea. When they become routine practice, caretakers will act
quickly at the first sign of diarrhoea, rather than waiting before treating the
child. The aim is that the recommendations become routine practice both in the
home and health-care facility.
MOTHERS AND OTHER CAREGIVERS SHOULD
- Prevent dehydration through the early administration of increased amounts of
appropriate fluids available in the home, and ORS solution, if on hand
- Continue feeding (or increase breastfeeding) during,
and increase all feeding
after the episode
- Recognize the signs of dehydration and take the child to a health-care provider
for ORS or intravenous electrolyte solution, as well as familiarize themselves
with other symptoms requiring medical treatment (e.g., bloody diarrhoea)
- Provide children with 20 mg per day of zinc supplementation for 10–14 days (10 mg
per day for infants under six months old).
HEALTH-CARE WORKERS SHOULD4
- Counsel mothers to begin administering suitable available home fluids immediately
upon onset of diarrhoea in a child
- Treat dehydration with ORS solution (or with an intravenous electrolyte solution
in cases of severe dehydration)
- Emphasize continued feeding or increased breast-feeding during, and increased
feeding after the diarrhoeal episode
- Use antibiotics only when appropriate, i.e. in the
presence of bloody diarrhoea
or shigellosis, and abstain from administering anti-diarrhoeal drugs
- Provide children with 20 mg per day of zinc supplementation for 10–14 days (10 mg
per day for infants under six months old)
- Advise mothers of the need to increase fluids and
continue feeding during future
episodes.
Health-care workers treating children for diarrhoea are encouraged to provide
caretakers with two 1-litre packets of the new ORS, for home-use until the
diarrhoea stops. Caretakers should also be provided with enough zinc supplements
to continue home treatment for 10–14 days. Printed material (including text and
illustrations) with advice on preventing and treating diarrhoea at home should
accompany the ORS and zinc supplements.
COUNTRIES SHOULD
- Develop a 3–5 year plan to reduce mortality rates
from diarrhoeal diseases
- Assess progress in controlling diarrhoeal diseases by
monitoring usage rates of
ORT/ORS, home-based treatment and zinc supplementation
- Using the media and face-to-face communication, promote and refine messages on
diarrhoea prevention, home management of diarrhoea and appropriate care-seeking
- Prioritize improving the availability of the new ORS
solution and zinc
supplements through private and public channels
- Craft suitable strategies to educate health-care workers at all levels about
using the new ORS and zinc supplements in treating diarrhoea
- Promote the availability of a zinc formulation that is
cost-effective and easily
administered to both infants and children
- Identify obstacles to the use of ORS, zinc supplements and home-based treatments
in managing acute diarrhoea.
UNICEF, WHO AND OTHER PARTNERS WILL SUPPORT THESE ACTIONS BY
- Advocating, facilitating and investing resources to
ensure country adoption and
implementation of these revised recommendations
- Working with governments and the private sector, including non-governmental
organizations and businesses, to rapidly disseminate these recommendations
-
Supplying new ORS and zinc supplements to countries that
cannot manufacture them to quality standards
-
Helping with communication efforts aimed at enhancing prevention and management
of diarrhoea, including promoting routine use of new ORS and zinc supplements.

Joy Phumaphi
Assistant Director General
Family and Community Health
World Health
Organization
Geneva |
Joe Judd
Director
Programme Division
United Nations Children’s Fund
New York |
REFERENCES
- Department of Child and Adolescent Health and Development, World Health
Organization, ‘Reduced osmolarity oral rehydration salts (ORS) formulation –
Report from a meeting of experts jointly organized by UNICEF and WHO’ (WHO/FCH/CAH/01.22),
New York, 18 July 2001
- Bahl, R., et al., ‘Effect of zinc supplementation on clinical course of acute
diarrhoea‘ – Report of a Meeting, New Delhi, 7-8 May 2001. Journal of Health,
Population and Nutrition,vol. 19, no. 4, December 2001, pp. 338-346.
- Bhutta Z.A., Black, R.E., Brown K. H., et al., ‘Prevention of diarrhoea and
pneumonia by zinc supplementation in children in developing countries: Pooled
analysis of randomized controlled trials’, Zinc Investigators’ Collaborative
Group, Journal of Paediatrics,vol. 135, no. 6, December 1999, pp. 689-697.
- For more details on the management of acute diarrhoea, consult ‘The Treatment of
Diarrhoea – A manual for physicians and other senior health workers’, WHO/CAH/03.7,
World Health Organization, Geneva.
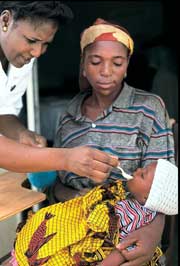
PHOTO CREDITS: Cover: A young Bangladeshi mother helps her healthy baby to
stand, © UNICEF/HQ93-1880/Shamsuz Zaman; Page 3: A health-care worker
spoon-feeds an ORS solution to a sick infant in the paediatrics ward of Kaduna
Hospital, Nigeria, © UNICEF/HQ97-1147/Giacomo Pirozzi
TECHNICAL ANNEX
ADVANCES IN MANAGING DIARRHOEAL DISEASES
NEW AND IMPROVED ORS WILL SAVE MORE LIVES
For more than 25 years, WHO and UNICEF have recommended a single formulation of
glucose-based ORS to prevent or treat diarrhoeal dehydration, no matter the
cause or affected age group. This solution has played a major role in
dramatically reducing global mortality due to diarrhoea. During this time,
researchers sought to develop an ‘improved’ ORS formulation that was as safe and
effective as the original in preventing and treating diarrhoeal dehydration but
also reduced stool output or offered additional clinical benefits, or both.
One research effort focused on reducing the osmolarity of ORS solution to avoid
possible adverse effects of hypertonicity on net fluid absorption. Reducing the
concentrations of glucose and salt (NaCl) in the solution accomplished this
goal. Studies of this approach show that decreasing the sodium concentration of
the ORS solution to 75 mEq/l, the glucose concentration to 75 mmol/l, and the
total osmolarity to 245 mOsm/l improved the efficacy of the ORS regimen for
children with acute non-cholera diarrhoea.
The need for unscheduled supplemental intravenous therapy in children given the
new ORS fell by 33 per cent. An analysis of this and other recent studies of
reduced osmolarity ORS solutions (osmolarity 210-268 mOsm/l, sodium 50–75 mEq/l)
found that stool output decreased by about 20 per cent and vomiting by about 30
per cent. The reduced osmolarity (245 mOsm/l) solution also appeared to be as
safe and effective as standard ORS for use in children with cholera.
RECOMMENDED FORMULATION
Because of the improved effectiveness of reduced osmolarity ORS solution,
especially for children with acute, non-cholera diarrhoea, WHO and UNICEF are
recommending that countries manufacture and use the following formulation in
place of the previously recommended ORS solution.
COMPOSITION OF REDUCED OSMOLARITY ORS
| Reduced osmolarity ORS
|
grams/litre |
| Sodium chloride |
2.6 |
| Glucose, anhydrous |
13.5 |
| Potassium chloride |
1.5 |
| Trisodium citrate, dihydrate |
2.9 |
| Total weight |
20.5 |
| |
|
| Reduced osmolarity ORS |
mmol/litre |
| Sodium |
75 |
| Chloride |
65 |
| Glucose, anhydrous |
75 |
| Potassium |
20 |
| Citrate |
10 |
| Total osmolarity |
245 |
|
ZINC SUPPLEMENTS REDUCE THE SEVERITY AND
DURATION OF DIARRHOEA
Twelve studies examined the impact of zinc supplements on the management of
acute diarrhoea. Eleven of these showed a reduction in the duration of the
diarrhoeal episode; in eight of these, the reduction was statistically
significant.
Five of the above studies also collected data on stool volume or frequency, and
found that zinc supplements reduced stool output or frequency. The data shows
that zinc supplementation during and until cessation of diarrhoea (either syrup
containing 20 mg of elemental zinc per 5 ml, or tablets of 20 mg zinc such as
zinc sulphate, gluconate or acetate) has a significant and beneficial impact on
the clinical course of acute diarrhoea, reducing both its duration and severity.
ZINC SUPPLEMENTS PREVENT SUBSEQUENT EPISODES OF DIARRHOEA
Other studies evaluating the effect of zinc supplementation on diarrhoeal
diseases found a preventive and long-lasting impact. These studies show that 10
mg to 20 mg of zinc per day for 10–14 days reduced the number of episodes of
diarrhoea in the 2–3 months after the supplementation regimen.
WHO and UNICEF therefore recommend daily 20 mg zinc supplements for 10–14 days
for children with acute diarrhoea, and 10 mg per day for infants under six
months old, to curtail the severity of the episode and prevent further
occurrences in the ensuing 2-3 months.
Printed May 2004
© The United Nations Children’s Fund/World Health Organization,
2004
This document may be freely reviewed, abstracted, reproduced and
translated,
but it cannot be sold or used for commercial purposes.
Ordering code: WHO/FCH/CAH/04.7
or UNICEF/PD/Diarrhoea/01
Copies of this statement and further information may
be requested from:
|
 World Health Organization World Health Organization
Department of Child and Adolescent Health and Development
Family and Community Health
20 Avenue Appia
1211 Geneva 27
SwitzerlandTel: 41-22-791-3281
Fax: 41-22-791-4853
Email: [email protected]
www.who.int
|
 United Nations Children's Fund United Nations Children's Fund
Health Section, Programme Division
3 United Nations Plaza
New York, NY 10017
USA
Tel: 1-212-326-7554
Fax: 1-212-303-7924
www.unicef.org
|
|