FAQ SHEET 1
Updated April 2004
HIV passes via breastfeeding to about 1 out of 7 infants born to HIV-infected women. But in many
situations where there is a high prevalence of HIV, not breastfeeding
dramatically increases the risk of infant mortality. Infants can die from
either the failure to appropriately breastfeed or from the transmission of HIV through breastfeeding.
In many programs to prevent mother-to-child transmission of HIV, the emphasis to date has
been on the provision of antiretroviral drugs to prevent transmission
around the time of delivery. Programs need to expand coverage and provide
mothers with information, guidance, and support that allows them to choose and adhere to the
safest infant feeding strategy for their situation.
 How many
infants are at risk of HIV? How many
infants are at risk of HIV?
Risk to infants of HIV-infected mothers.
In the absence of any intervention, between 15 and 30 percent of infants of HIV-infected mothers are infected before or
during delivery. If all HIV-infected mothers breastfeed, another 10 to 20 percent of their infants will be infected through
breastfeeding. This means that about two-thirds of children of HIV-infected women will not become infected.
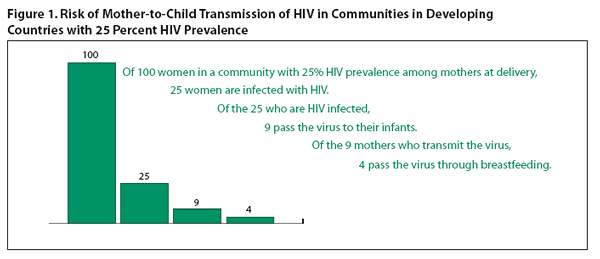
Risk to all infants in a community.
Although the percentage of mothers infected with HIV approaches 40 percent in some African communities, it generally
is much lower, rarely above 25 percent (one in four).
The risk of HIV transmission via breastfeeding can be calculated by multiplying the HIV prevalence rate among mothers at the time of
delivery (25 percent in the example below) by 15 percent (25 percent at risk x 15 percent infected through breastfeeding =
3.75 percent). In other words, even where 25 percent of women are infected with HIV and all of them breastfeed, less than 4 percent of all infants in the
community will be infected through breastfeeding.
 Does breastfeeding pose any risk to the HIV
-infected mother? Does breastfeeding pose any risk to the HIV
-infected mother?
Only two studies have examined the association between breastfeeding and the health of HIV-infected mothers, and their
findings were contradictory. WHO reviewed these studies, concluded that the results did not merit a change in current recommendations,
and urged more research on the topic.
All mothers should increase their food intake and eat nutrient-rich food during lactation. Breastfeeding uses energy and other
nutrients that need to be replaced to keep a mother healthy. Nutritional support is particularly important for the
HIV-infected mother because HIV puts an additional strain on her energy and nutrient stores and may affect her
appetite.
 Should mothers with HIV be advised not to breastfeed? Should mothers with HIV be advised not to breastfeed?
IT DEPENDS . . .
IF a mother knows she is infected, and
IF breastmilk substitutes are affordable and can be fed safely with clean water, and
IF adequate health care is available and affordable,
THEN the infant’s chances of survival are greater if fed artificially.
HOWEVER,
IF infant mortality is high due to infectious diseases such as diarrhea and pneumonia, or
IF hygiene, sanitation, and access to clean water are poor, or
IF the cost of breastmilk substitutes is prohibitively high, or
IF access to adequate health care is limited,
THEN breastfeeding may be the safest feeding option even when the mother is HIV-positive.
Even where clean water is accessible, the cost of locally available formula exceeds the average household’s income.
If families cannot buy sufficient supplies of breastmilk substitutes, they may:
- over-dilute the breastmilk substitute,
- under-feed their infant, or
- replace the breastmilk substitute with dangerous alternatives.
In the 50 poorest developing countries, infant mortality averages over 100 deaths per thousand live births.
Artificial feeding can triple the risk of infant death.
 If a mother with HIV breastfeeds, how can she reduce the risk of transmission? If a mother with HIV breastfeeds, how can she reduce the risk of transmission?
HIV-positive women may be able to reduce the risk of transmission by:
- Breastfeeding exclusively for the first six months.
Many experts believe that the safest way to breastfeed in the first six months is to do so exclusively, without
adding any other foods or fluids to the infant’s diet. These additions are not needed and may cause gut infections
that could increase the risk of HIV transmission. In South Africa, HIV-positive mothers who reported breastfeeding exclusively
for at least three months were less likely to transmit the virus to their infants than mothers who introduced
other foods or fluids before three months. Moreover, their risk of transmitting the virus was no greater
than among mothers who never breastfed.
- Shortening the total duration of breastfeeding.
There is evidence that the risk of transmission continues as long as the infant is breastfed. The risk of
death due to replacement feeding (feeding an infant who is not receiving any breastmilk a nutritionally adequate diet) is
greatest in the first few months and becomes lower over time. As the infant ages, a breastfeeding mother should
reassess her situation and the risk factors associated with various feeding options. If replacement feeding
becomes acceptable, feasible, affordable, sustainable, and safe, she should transition to replacement feeding. The
optimum time and strategy for introducing substitutes is not known and varies with the situation. Under conditions
common in resource-limited settings, many experts recommend a transition from exclusive breastfeeding to
replacement feeding at about 6 months of age.
- Preventing and promptly treating oral lesions and breast problems.
If an infant has oral lesions (commonly caused by thrush) or if a mother has breast problems such as cracked nipples or mastitis, the risk of transmission is higher.
- Taking antiretroviral drugs. In a clinical trial in Uganda, a single
dose of nevirapine to a mother during labor and another to her infant after delivery reduced transmission in
breastfed infants by 42 percent through six weeks and by 35 percent through 12 months. The simplicity and lower
cost of the nevirapine regimen—compared with other regimens that are prohibitively expensive for most poor
households—offers hope that it will become an important component of programs to reduce mother-to-child transmission.
Many studies are now underway to find out if antiretroviral drugs used by the mother or the infant during the
breastfeeding period can further reduce transmission. The safety and effectiveness of these regimens are not yet known.
 What are he current international recommendations on breastfeeding and HIV? What are he current international recommendations on breastfeeding and HIV?
The latest UN policy statement on HIV and infant feeding was issued in 2001, following an expert consultation on mother-to
child transmission of HIV. Regarding the balance of risks between breastfeeding and replacement feeding, the statement says:
“When replacement feeding is acceptable, feasible, affordable, sustainable, and safe, avoidance of all breastfeeding by HIV
infected mothers is recommended. Otherwise, exclusive breastfeeding is recommended during the first months of life. To
minimize HIV transmission risk, breastfeeding should be discontinued as soon as feasible, taking into account local
circumstances, the individual woman’s situation, and the risks of replacement feeding (including infections other than
HIV and malnutrition). When HIV-infected mothers choose not to breastfeed from birth or stop breastfeeding later, they should
be provided with specific guidance and support for at least the first 2 years of the child’s life to ensure adequate
replacement feeding. Programmes should strive to improve conditions that will make replacement feeding safer for
HIV-infected mothers and families.”
The statement emphasizes the need for counseling on the risks and benefits of different feeding options but recognizes that
“many women find that receiving information on a range of infant feeding options is not sufficient to enable them to choose and
they seek specific guidance.”
To help countries implement this policy, guidelines for policy makers and health care managers were published by the UN
agencies in 1998 and updated in 2003. Most countries offer voluntary counseling and testing as part of antenatal
services. Pregnant women who test positive for HIV receive counseling on infant feeding options, among other
things. To understand all the positive and negative effects on feeding practices and infant health among HIV-positive
mothers and in the general population, it is important that these efforts are adequately monitored and evaluated.
The International Code of Marketing of Breastmilk Substitutes was introduced by the World Health Organization in
1981 to counter the negative effects of the introduction of breastmilk substitutes in developing countries. The Code’s
provisions are particularly relevant in this era of HIV and should continue to be promoted and observed. The effects of a
general reduction in breastfeeding would be disastrous for child health and survival.
 What population-based strategies can promote breastfeeding and minimize HIV transmission? What population-based strategies can promote breastfeeding and minimize HIV transmission?
Promote safer sexual behavior.
The best way of protecting children from HIV is to help women avoid HIV infection. Most infection is through unprotected
sexual intercourse. The risk of infection can be lowered by decreasing the number of sexual contacts, reducing the number of
partners, and using condoms. Methods of protection that women themselves can control are urgently needed. Treating and preventing other sexually
transmitted diseases can also help decrease the risk of HIV transmission. Improving the economic and social conditions of women and girls also would
reduce their vulnerability to coercive and other unsafe sexual situations.
Provide universal access to voluntary and confidential HIV testing and counseling for both men and women.
At present, access to HIV testing is generally low, yet many of the strategies proposed for reducing mother-to child transmission assume that
the mother’s HIV status is known. Even where testing is available, mothers often do not want to know their status or cannot be
assured that test results will be confidential.
Communicate the advantages of knowing one’s HIV status.
As treatment, care, and support for people living with AIDS become more effective and available, the advantages of knowing one’s status will
increase. If a mother knows she is infected, she can try to minimize the risk of transmission to her partners and children and, if she chooses, avoid further
pregnancies. As part of her counseling, she should be given information on the risks and benefits of infant feeding options. If she knows she is not
infected, she should be counseled to breastfeed, knowing that there is no risk of infecting her child. She should also be motivated to protect herself from
further risk of infection. Stimulating demand for testing by emphasizing these advantages along with ensuring the availability of confidential testing is essential.
Provide technical information to opinion makers.
Health care providers and groups with public influence— such as the media, policy makers, and health advocates— need
accurate technical information on this issue to prevent the spread of misinformation and to maintain the strength and credibility of
breastfeeding promotion activities.
Provide locally adapted counseling guidelines to health workers.
UN agencies have developed counseling guidelines for health workers and policy makers that address the risks and
benefits of available infant feeding methods and how to make the chosen method of infant feeding as safe as possible.
These guidelines need to be adapted to reflect local conditions and feasible infant feeding alternatives.
Train health workers to counsel mothers.
Locally adapted guidelines are not enough by themselves to ensure that mothers’ infant feeding decisions are well
informed. It takes skill, experience, sensitivity, and understanding to assess a mother’s situation and to
communicate all the information that she needs (on modes of transmission, risk factors, preventive strategies, and the
level of health service support available) to balance the risks and benefits of feasible infant feeding strategies.
Continue to promote, protect, and support breastfeeding.
In the absence of breastfeeding promotion, there is a danger that information about HIV transmission during
breastfeeding will result in inappropriate discontinuation of breastfeeding among both HIV-positive mothers and
uninfected mothers who do not know their status. Breastfeeding promotion should include continued efforts to monitor the
observance of the provisions of the International Code of Marketing of Breastmilk Substitutes and the use and
misuse of information on breastfeeding and HIV.
Support research.
Policies and programs remain hampered by uncertainty. We need to know more about factors that influence transmission rates and about the risks
associated with different feeding alternatives at different ages in poor environments. There is a particular need to distinguish
different patterns of breastfeeding using standard definitions. We also need to translate this information into knowledge that the mother can use to make
the best infant feeding decision for herself, her baby, and her family.
 What advice can health workers give to mothers? What advice can health workers give to mothers?
Each situation is unique, and health workers must tailor their advice to the individual needs of each mother. Ultimately, the
infant feeding choice is the mother’s, but this decision should be based on the best information available. The
role of the health worker is to provide this information and the support needed to make the mother’s choice as safe as
possible. Box 1 offers counseling guidelines for various situations.
For the woman who is not infected, breastfeeding is clearly the best choice. Breastfeeding remains one of the most effective
strategies to improve the health and chances of survival of both the mother and child. It provides a complete and hygienic
source of the infant’s fluid and nutritional requirements through the first six months of life, as well as growth factors and
antibacterial and antiviral agents that protect the infant from disease for up to two years and more. Breastfeeding also contributes to child spacing
and women’s longterm health. These benefits of breastfeeding are likely to be even greater in emergency situations
where safe preparation and use of breastmilk substitutes may be more difficult that in normal circumstances.
References
Coutsoudis A, Pillay K, Kuhn L, et al. Method of feeding and transmission of HIV-1 from mothers to children by 15 months of age: prospective
cohort study from Durban, South Africa. AIDS 15:379-387, 2001.
De Cock KM, Fowler MG, Mercier E, et al. Prevention of mother-to-child HIV transmission in resource-poor countries: Translating research
into policy and practice. JAMA 283:1175-1182, 2000.
Gaillard P, Fowler M-G, Dabis F, et al. Use of antiretroviral drugs to prevent HIV-1 transmission through breast-feeding: From animal
studies to randomized clinical trials. J Acquir Immune Defic Syndr 35:178-187, 2004.
Preble EA, Piwoz EG. Prevention of Mother-to-Child Transmission of HIV in Asia: Practical Guidance for Programs. A joint
publication of the LINKAGES and Support for Analysis and Research in Africa (SARA) Projects. Academy for Educational Development: Washington, DC: 2002.
Ross JS, Labbok MH. Modeling the effects of different infant feeding strategies on young child survival and mother-to-child transmission
of HIV. Am J Pub Health 2004 (in press).
WHO Technical Consultation on Behalf of the UNFPA/UNICEF/WHO/UNAIDS Inter-Agency Task Team on Mother-to-Child Transmission of HIV. New Data on
the Prevention of Mother-to-Child Transmission of HIV and Their Policy Implications: Conclusions and Recommendations.
WHO/RHR/01.28. World Health Organization: Geneva, 2001.
WHO. HIV and Infant Feeding: Framework for Priority Action. World Health Organization: Geneva, 2003.
WHO/UNAIDS/UNICEF. HIV and Infant Feeding: Guidelines for Decisionmakers. World Health Organization: Geneva, 2003.
WHO/UNAIDS/UNICEF. HIV and Infant Feeding: A Guide for Health Care Managers and Supervisors. World Health Organization: Geneva, 2003.
This FAQ Sheet is a publication by LINKAGES: Breastfeeding, LAM, Complementary Feeding, and Maternal Nutrition Program, and was made possible through support
provided to the Academy for Educational Development (AED) by the Bureau for Global Health of the United States Agency for International Development (USAID), under the
terms of Cooperative Agreement No. HRN-A-00-97-00007-00. The opinions expressed herein are those of the authors and do not necessarily reflect the views of USAID.
|