|
| |
Issue no. 55 - December 1993-February 1994
pdf
 version of this Issue version of this Issue
|
There is much information in this issue that is valuable
and useful. Online readers are reminded, however, that treatment guidelines and health
care practices change over time. If you are in doubt, please refer to
WHO's up-to-date Dehydration Treatment
Plans.
|
updated: 23 April, 2014
Pages 1-8 Dialogue on Diarrhoea Online Issue 55 - December
1993-February 1994
|
Dialogue
on Diarrhoea Issue no. 55 December
1993-February 1994  Page 1 2
Page 1 2
Breaking the drug habit
Medicinal drugs can be life-saving. They
have a valuable, but limited, role in the management of some diarrhoeal diseases such as
bloody diarrhoea - the subject of a special supplement in this issue. However, even the
best drugs can sometimes have unwanted and even harmful side-effects. DD discusses ways to limit the use of unnecessary drugs in diarrhoea
management. There are several different approaches to combating inappropriate use of
drugs. These include: laws and regulations: educating health professionals; and campaigns
to raise public awareness. Consumer groups and health campaigners can alert the government, health workers and the
public to misuse of medicinal drugs. This can result in laws or regulations banning the
sale of harmful drugs, or removing these drugs from the lists of drugs distributed to
government health facilities. This happened with anti-diarrhoeals in the Philippines (page 4) and with paediatric formulations of loperamide - an
anti-diarrhoeal that caused the deaths of several infants in Pakistan (page
5).
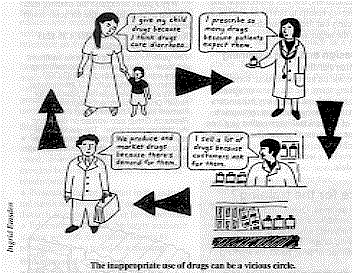 |
The
inappropriate use of drugs can he a vicious circle. Can laws against misuse of drugs be enforced? Unless legal action is supported by
health workers and the public, then selling of harmful drugs may continue. Health workers
need to be trained in the rational use of drugs - how to give the right drug to the right
child at the right time.
|
Doctors are not the only people who prescribe drugs. In many countries, when someone is
ill, families turn first to their local pharmacy or drug store for advice and treatment.
This has been recognised by WHO which has designed a training course for people who sell
drugs in the private sector (page 2). The general public also needs to know what drugs can and cannot do. People's
expectations of the power of drugs have been raised by the discovery of antibiotics that
can treat bacterial infections such as meningitis and pneumonia. Many people now believe
in a 'pill for every ill', and demand drugs for diarrhoea. However, most childhood
diarrhoea is caused by viruses, not treatable with antibiotics. Except for specific cases
- such as bloody diarrhoea and cholera with severe dehydration - drugs will not help
diarrhoea. With oral rehydration therapy and good feeding, most children will recover well
from diarrhoea. Check your own practice. Are you prescribing unnecessary drugs for diarrhoea? Are local
shops and pharmacies near you major providers of advice about diarrhoea? Would they be
willing to join a suitable training programme? Can you do anything to limit the ordering
of unnecessary drugs in your health centre or hospital? William Cutting and Katherine Elliott
|
|
Dialogue
on Diarrhoea Issue no. 55 December
1993-February 1994  1 Page 2 3 1 Page 2 3
Educating drug sellers
Drug stores are often the first places people go to for medical advice. Robert
Hogan describes a WHO guide to training private sector pharmacists and drug
sellers. When trying to improve management of
diarrhoea, it is important to work with all providers of care, not just the government
health system. Many ministries of health run training programmes to improve the way doctors, nurses
and community-based health workers manage diarrhoea; but until recently little attention
has been paid to private sector drug sellers.
| In most
countries, private sector pharmacies and over-the-counter drug stores are a common source
of advice on health matters. Pharmacies and drug stores are more widespread than public
health facilities and are often the first place people go to when they or their children
are sick. |
|
 |
But advice given to
customers about diarrhoea and products sold are usually inappropriate, and sometimes
dangerous. Ineffective anti-diarrhoeal drugs are frequently recommended instead of oral
rehydration therapy. |
Reasons for this include: lack of knowledge; availability of inappropriate drugs;
consumer demand for drugs; inappropriate prescribing by doctors: higher profit margins for
anti-diarrhoeal drugs than for ORS; and drug regulations that do not encourage rational
use of drugs. Ideally, a diarrhoeal disease control (CDD) programme would tackle all these factors.
But many countries do not have the resources for such a comprehensive strategy. As a first
step, WHO has designed a training approach focusing on one key area - improving drug
sellers' knowledge. The approach combines face-to-face communication (trainers meet with drug sellers
individually or in small discussion groups), with distribution of printed material (such
as pamphlets and posters) promoting correct practice. A training manual has been
field-tested in Kenya (see="#page4">page 4) and Indonesia. It provides a
step-by-step guide to setting up a training programme relevant to local needs. The following steps are suggested. 1. Learn about how drug sellers treat diarrhoea and why
- Study the system for drug sales: identify drug outlets and sellers; identify the
top-selling ORS and anti-diarrhoeal drugs.
- Choose a target audience: identify which type of drug outlet and geographical area to
target.
- Use a survey to learn about what drug sellers already know and do.
- Identify factors that influence drug sellers' practices: consult local experts such as
the pharmacists' association, the Ministry of Health, pharmaceutical manufacturers; use
this information and the survey results to devise key questions and carry out focus group
discussions with the target audience.
2. Design and plan a training intervention
- Decide on an intervention: form a working team; use the research already done to work
out which key behaviours to change; choose the most appropriate type of educational
intervention (e. g. one- to-one visits, small group discussions, see="#page3">page
3).
- Develop a workplan, including a time schedule.
- Develop printed materials: choose main messages based on earlier research; design
materials; pre-test (show the materials to selected people from the target audience, to
assess their reaction).
- Train the trainers and pilot test the educational intervention.
3. Carry out the intervention and evaluate results
- Develop a plan for monitoring and evaluation of the training.
- Implement and assess the intervention.
The two field tests have shown that lack of knowledge and skills are important reasons
why drug sellers behave as they do. Training that changes knowledge and skills can change
behaviour, at least initially. WHO plans to expand the training intervention to include drug use for acute respiratory
infections. Robert Hogan, CDR, WHO, CH-1211 Geneva 21, Switzerland. The guide for improving diarrhoea treatment practices of pharmacists and licensed
drug sellers was produced by the WHO CDD programme together with ACT International,
Atlanta and the Management Sciences for Health Drug Management Programme. Harvard Medical
School's Drug Policy Research Group also worked on designing the training intervention.
The guide is available to national CDD programmes or other organisations training
pharmacists and drug sellers. Write to COD, WHO, CH-1211 Geneva 27, Switzerland.
|
Who is the target audience for the training?
Drugs are sold in a wide variety of commercial settings. Outlets include pharmacies,
over-the-counter drug stores, supermarkets, variety stores, small neighbourhood shops,
kiosks and peddlers. The WHO educational intervention is aimed at outlets whose main
business is selling drugs. Field tests concentrated on pharmacies. The intervention is not
aimed at drug peddlers working in the informal sector. Staff who work in drug outlets vary from country to country - they include:
- pharmacists who are graduates of university degree programmes
- assistant pharmacists who often have post-secondary school diplomas
- dispensers who have focal training and have served a technical apprenticeship
- sales clerks who are usually literate, but have no formal training.
|
|
DDOnline Dialogue
on Diarrhoea Online Issue no. 55 December
1993-February 1994  2 Page 3 4 2 Page 3 4
A choice of training methods
The WHO guide describes three main approaches to training drug sellers. Different
methods will suit different local circumstances and resources. One-to-one education Health education studies and over 100 years' experience of commercial drug marketing
show that visits by educators to drug stores and pharmacies can be a very effective way to
change the behaviour of staff who work in them.
 |
This
approach is sometimes called 'educational outreach'. Trained educators from respected
organisations (such as professional associations, universities or ministries of health)
visit drug sellers to offer objective advice and give support for improving treatment
decisions. Educators should plan two visits to each drug seller targeted. On the fist visit the
educator describes the different types of diarrhoea, then discusses with the drug seller
the causes and treatment of dehydration, and the advantages and disadvantages of different
drugs.
|
Specific, easy-to-remember recommendations are emphasised and reinforced at the
beginning and end of each visit. Printed educational materials are left with the drug
seller to be pinned on a wall or kept for reference on the counter or desk. A single visit is unlikely to bring about lasting change. A follow-up visit should be
made to remind the drug seller about key messages, and to allow discussion of practical
problems (for example, how to overcome customer demand for antibiotics). Strengths
- One-to-one training approaches are more memorable to the person being educated, so
important facts and recommended behaviours are more likely to be remembered.
- Education can be targeted to the individual needs and problems of each drug seller
through discussion of his or her experience.
- Educators can reach the target audience at their workplaces without having to persuade
them to travel to a meeting.
Weaknesses
- The costs of visiting every targeted drug store may be high. It may be difficult for a
few educators to contact drug sellers in a widely dispersed area.
- There may not be a quiet place in the store for an uninterrupted discussion, and there
may not be enough time for a good discussion.
Small group discussions
|
Groups
of six to eight drug sellers are invited to an informal meeting for a presentation by a
trained educator followed by a discussion. The meeting lasts1-2 hours and should take place in a quiet place close to the drug
sellers' workplaces. Incentives such as snacks could be provided to encourage
participation.
|
 |
Strengths
- It costs less since 6-8 people are educated in one meeting.
- Drug sellers may find it easier to speak honestly about their practices in the presence
of other participants from a similar background.
- Better informed participants may influence others to change their behaviour.
Weaknesses
- It may be difficult to persuade people to take time off work to attend a meeting. More
co-ordination is required to get everyone to the same meeting.
- Drug sellers may feel a sense of competition and not want to co-operate in a group.
- The person attending the meeting may not be the person selling ORS or drugs, and they
may not take the message back to their colleagues or staff.
Larger training seminars Some health professions already organise continuing education programmes. Similarly,
groups of 10-30 pharmacists and drug sellers could be invited to a large formal training
seminar. After a presentation, participants could break into small groups to discuss
particular topics. Strengths
- Many organisations already have experience of conducting large training seminars.
Respected experts may be willing to address a session.
- Trainers reach a greater number of people at one time, so less time and money is
required.
Weaknesses
- Drug sellers who most need to change their practice may not attend.
- Achieving active participation in large meetings is more difficult.
- Messages cannot easily be targeted to individual problems.
|
|
DDOnline Dialogue
on Diarrhoea Online Issue no. 55 December
1993-February 1994  3 Page 4 5 3 Page 4 5
Working with pharmacists in Kenya Pradeep Goel, Joseph Makhulo and Gitau Mwangi
describe Kenya's experience of field-testing a WHO guide on training private sector
pharmacists. A typical urban retail pharmacy in Kenya
is visited by anywhere between 10 and 99 customers a day with health problems but no
prescription from a doctor. In small towns with fewer doctors, the number may be even
greater. Kenya's diarrhoeal disease control (CDD) programme used the WHO guide (page
2) to carry out a training programme to improve advice given by pharmacists and their
assistants about managing diarrhoea. From the start, the CDD programme involved the Pharmaceutical Society of Kenya, the
Kenya Medical Training Center and the University of Nairobi. Kenya's capital, Nairobi, and five other towns were chosen as sites for the training
programme. The range of training methods included: one-to-one discussions with an opinion
leader within a pharmacy (e. g. pharmacy owners); one-to-one discussions with pharmacists;
and small group training sessions for pharmaceutical assistants.
|
Kenya's poster message Four types of printed materials were used after pre-testing: two pamphlets for pharmacy
staff (one on ORS and the other on anti-diarrhoeals); a general pamphlet for customers;
and a wall poster. Small group training sessions were found to be the most effective method because,
unlike in large seminars, attention could be paid to individual needs. Importantly, small
groups allowed discussion of constraints in applying recommendations. Role plays on
advising customers were acted out.
|
 |
The pilot phase of the training has been completed: 162 pharmaceutical assistants in 90
pharmacies have received training. Initial evaluation shows promising results.
Questionnaires given to participants before and after training showed that training
increased overall knowledge. Purchase surveys in five towns showed that ORS sales
increased by 24-32 per cent, while sales of anti-diarrhoeals decreased by 6-12 per cent. Several lessons can be learnt from Kenya's experience.
- It is important to find out why drug sellers behave as they do. In some cases, drug
sellers may have adequate knowledge, but motivation may be the problem. Working out what
sort of training will best meet the needs identified is also crucial.
- Pharmacy staff prefer the training to come from an independent and credible organisation
(such as WHO or UNICEF). The training should not appear as a threat. It is important to
involve the professional association of pharmacists. The involvement of organisations and
individuals outside the CDD programme is vital.
- Producing printed materials is one of the most expensive parts of the intervention.
Therefore, only one or two carefully designed printed materials should be used to convey
the training messages.
Dr Pradeep Goel, Dr Joseph Makhulo and Dr Gitau Mwangi, C/ o Drug Management
Programme, MSH, 165 Allandale Road, Boston MA 02130, USA.
Regulation plus education Elvira Dayrit and Juanita
Basilio report on tough action in the Philippines to curb the
irrational use of drugs. A household survey in 1987 in the
Philippines showed that drugs were used in at least 55 per cent of cases of childhood
diarrhoea. The Department of Health was the biggest purchaser and user of
anti-diarrhoeals. As a result of these findings, major changes were made to the systems of drug
procurement and distribution in 1988-9. The purchase and prescription of anti-diarrhoeals in government health facilities were
banned. Amoebicides were delisted from regular government procurement lists and can now
only be prescribed after laboratory diagnosis. All paediatric forms of loperamide and
diphenoxylate were deregistered by the Philippine Bureau of Food and Drugs, effectively
banning them from both private sector drug stores and government health facilities.
Requirements for registration were made more difficult for all anti-diarrhoeals.
Advertising of loperamide to the general public was also banned. As well as legal changes, an educational campaign for doctors, nurses and pharmacists
was launched. A national workshop involving a range of health organisations resulted in
the following activities:
- Pharmacology, microbiology, parasitology and pathology departments belonging to the
Association of Philippines Medical Colleges developed curricula to promote rational drug
use.
- Philippines Medical Association chapters held workshops; conducted outreach education
activities for families; showed films in hospitals; and organised media campaigns on oral
rehydration therapy. .
- The Philippine Pharmaceutical Association incorporated 'responsible dispensing in acute
diarrhoea' in their continuing education programmes for community pharmacists.
- Several NGOs held seminars on rational drug use. Volunteer community health workers of
these NGOs also received training on rational drug use.
Three years after the initial household survey, surveys in selected cities showed a
reduction in drug use for diarrhoea from 55 per cent of cases to 36 per cent. As a result
of tighter rules for drug registration. the number of anti-diarrhoeal brands on the market
was reduced from 206 brands in 1987 to 56 brands in 1992. The national action was successful because it was taken up by many different
organisations, not just the Department of Health. It also happened at a time when there
was widespread professional and political support to tackle drug misuse. Dr Elvira Dayrit and Dr Juanita Basilio, Maternal and Child Health Service,
Department of Health, San Lazaro Compound, Santa Cruz, Manila, The Philippines.
|
|
DDOnline Dialogue
on Diarrhoea Online Issue no. 55 December
1993-February 1994  4 Page 5 6 4 Page 5 6
North-south network
International campaigns to stop the promotion of dangerous drugs can be very
effective, as Catherine Hodgkin of Health
Action International explains.
 |
A nutritious diet and clean water are often the best 'medicines'. In 1981 health, development. consumer
and public interest groups around the world formed a network - Health Action International
(HAI) - to co-ordinate campaigns on drug issues and to facilitate exchange of information
internationally. Since then, the network has grown to include about 150 HAI member groups
in 60 countries.
|
Anti-diarrhoeal drugs were the target of HAI's first international campaign because of
their widespread inappropriate use. Over the past 12 years many HAI groups have been
actively involved in promoting oral rehydration and challenging the use of inappropriate
drugs. By working together internationally, groups within the network have made an impact
which individual groups could not have achieved. In 1990 British television screened a documentary showing how infants in a hospital in
Pakistan were dying of bowel paralysis caused by loperamide (Imodium). The programme also
highlighted the negative effects of bottle-feeding. The doctor featured in the
documentary, Professor Tariq Iqbal Bhutta, was a member of the HAI network and had been
active in drawing the world's attention to the problem. Following the TV programme, backed up by a campaign being waged by a number of
organisations internationally, paediatric formulations of loperamide were withdrawn
worldwide. Many countries, including Pakistan, took regulatory action to limit the
availability of anti-diarrhoeals. The press materials and briefing pack developed by HAI to follow up Professor Bhutta's
work resulted in studies on the use of anti-diarrhoeals in Finland, France and the UK. In
Bangladesh, an HAI member group undertook a major promotion of the WHO guidelines on
rational drug use. In India the TV film was used to train medical students. Next year the
film will be shown at CDD training courses in Vietnam. In Latin America, a campaign co-ordinated by the regional HAI network, Acción
International para la Salud (AIS) helped to achieve deregistration of anti-diarrhoeals in
Peru and Mexico. Groups belonging to AIS have produced educational materials for
prescribers and consumers, including treatment guidelines, posters, comic books for
children and a resource book for groups working against anti-diarrhoeals. Concern about the misuse of drugs for managing diarrhoea is also being voiced in the
United States where several anti-diarrhoeals in common use internationally are produced. A
US consumer group, Public Citizen, petitioned the US Food and Drug Administration (FDA) to
withdraw the licences of anti-diarrhoeals. The FDA was targeted not only because of the
problem of inappropriate use of drugs in the US, but also because a US licence is often
seen as a 'passport' to registration in other countries. The FDA is still considering the
petition but is likely to recommend changes in the licence provisions of several
anti-diarrhoeals. As well as involving member groups of its network, HAI frequently works in co-operation
with other organisations such as WHO, UNICEF, associations of health professionals and
other relevant groups such as the Medical Lobby for Appropriate Marketing (page 6). Catherine Hodgkin, Co-ordinator HAI Europe, Jacob van
Lennepkade 334-T, 1053 NJ Amsterdam, The Netherlands. Other HAI regional co-ordinating offices are: HAI Clearinghouse, c/ o IOCU, PO Box 1045, 10830 Penang, Malaysia.
AIS Latin America, Avda. Palermo 531, Dpto. 104, Lima 13. Peru.
Problem Drugs
- a campaign and information pack produced by HAI Problem Drugs (revised and updated in 1993) contains well-documented
and up-to-date information sheets on many types of drugs including anti-diarrhoeals. It
highlights examples of unethical marketing and gives clear recommendations for action. Available from: HAI Europe (see address="#HAI">above). Price: D. fl. 30
plus D. fl. 5 for postage. Reduced rates available for groups in developing countries, HAI
members and bulk orders. Please write for details.
|
Other organisations INRUD (International Network for Rational Use of Drugs) The International Network for Rational Use of Drugs (INRUD) is an organisation of
health professionals, administrators and researchers in developing countries who wish to
undertake innovative programmes to improve the use of drugs. INRUD provides a forum to
communicate, exchange information and ideas, co-ordinate research, develop human resources
and link projects with interested donors. The network links groups in both Africa and
Asia, including organisations in Nigeria, Ghana, Tanzania, Uganda, Zimbabwe, Nepal,
Bangladesh and Indonesia. For more information about INRUD, please contact: Dr Richard Laing, INRUD
Co-ordinator, Management Sciences for Health, 165 Allandale Road, Boston, MA 02130, USA.
|
|
DDOnline Dialogue
on Diarrhoea Online Issue no. 55 December
1993-February 1994  5 Page 6 7 5 Page 6 7
Successful campaign
Zafar Mirza explains how a campaign
against drug misuse in one country can lead to action in the rest of the world.
|
Irrational
drug use is widespread in Pakistan. The problems include: inefficient mechanisms for drug
registraton; lack of quality control of drugs; easy access to all types of drugs without
prescription; untrained sales staff at medical stores; inappropriate prescribing by
doctors; unethical drug promotion and misleading information by the pharmaceutical
industry, prescribing by quacks; and self-medication. Two years ago a group of concerned health workers and members of the public set up the
Network of Association for Rational Use of Medication in Pakistan, to try to combat drug
misuse.
|
 |
A founding member of the network, Professor Tariq Iqbal Bhutta, was already well known
internationally for his campaigning work against loperamide (see="#page5">page 5).
The network is working on documenting the campaign so that other countries can learn from
the experience. Campaigning against harmful drugs is still an important part of the network's work.
Last year, Piptal paediatric drops (pipenzolate bromide and phenobarbitone) were
deregistered following a network-led campaign. Piptal drops (promoted for treating colic in infancy) had been deregistered in 1990
along with loperamide. The drug combination in Piptal drops can cause abdominal distension
and sleepiness, and has been linked to the deaths of two infants in Pakistan. However, in
1991 the drops were re-registered following lobbying by the manufacturer. The network
alerted MaLAM (see below), and international pressure resulted in the
Ministry of Health deregistering the drops again. Through its quarterly newsletter, the network now reaches around 10,000 supporters. The
network's activities are wide-ranging - including education, information provision,
campaigning and research. The network recently received recognition from WHO and
Pakistan's Ministry of Health when it was asked to review the country's diarrhoeal disease
control programme. The network has become the best independent source of information about drugs in
Pakistan. An enquiry service to reply to members' requests for information on specific
drugs has recently been launched. The network plans to become involved in consumer
education next year. Irrational drug use is a complex problem, and Pakistan has made a step in the right
direction. It is important that drug use continues to be monitored and public awareness
raised. There is still a long way to go before rational drug use is a reality. Dr Zafar Mirza, The Network Co-ordinator, House no. 57, G-8/2, Islamabad, Pakistan. Countering misleading marketing
John Appleby reports on the Medical
Lobby for Appropriate Marketing (MaLAM), an international group campaigning for honest
advertising of medicines. Misleading advertising of drugs is a serious problem
worldwide. A survey of drug advertisements in five journals carried out by the Australian
Society of Clinical and Experimental Pharmacologists in 1985 and 1986 found that 31 per
cent of advertisements were misleading or contained unjustifiable claims. Although many doctors deny that advertising influences them, controlled trials have
shown that advertising techniques are more effective at influencing prescribing behaviour
than methods used in medical education. Misleading marketing is more common in Africa, Asia and Latin America than in
industrially developed countries. Yet in developing countries, where less money is
available for medicines, and mortality rates are relatively high, the need for accurate
information about appropriate use of drugs is greater. The Medical Lobby for Appropriate Marketing (MaLAM) was set up in 1983 to monitor drug
promotion and lobby for improved standards. MaLAM's headquarters are in Australia, but it
has members in more than 30 countries, and branches in seven countries. It works by providing information to subscribers (who are mainly, but not exclusively,
health workers) and encouraging them to question drug companies about specific promotional
practices. Supporters send in examples of misleading advertisements, and each month MaLAM sends a
letter to subscribers focusing on a particular drug. A form letter addressed to the
relevant drug company is included in the mailing. If the MaLAM subscriber agrees with the
letter, they are asked to sign it and send it directly to the company, asking for a
personal reply to a series of questions. Through this technique, a few minutes of each subscriber's time can put considerable
pressure on a drug company. Letter campaigns by MaLAM have had several successes,
including contributing to Upjohn promising to phase out the marketing of Kaomycin
(containing neomycin, kaolin and pectin) for acute diarrhoea in children by May 1992.
However, questionable advertisements are still appearing in some countries. Although many drug companies continue to make unjustifiable claims about their
products, health workers' awareness of the need for better information is growing.
Companies are beginning to realise that they have to use scientific evidence to support
claims about medicines or they will lose credibility with drug prescribers. John Appleby, Co-ordinator, MaLAM UK, 12 Hugill Street, Bradford BD13 3JW, UK.
Other branches of MaLAM include: MaLAM International HQ, PO BO. Y 172, Daw Park, SA 5041. Australia.
MaLAM-India, Siddartha Medical College, Vijayawda 520 008, Andhra Pradesh, India.
MaLAM-Pakistan, C/o Dr H Carmichael, Women's Christian Hospital, 85 Nusrat Road, Multan
CANT 60000. Pakistan.
MaLAM-Sri Lanka. C/ o SIRHA, Dept. of Pharmacology, Faculty of Medicine, Kinsey Road,
Colombo 8, Sri Lanka.
|
|
DDOnline Dialogue
on Diarrhoea Online Issue no. 55 December
1993-February 1994  6 Page 7 8 6 Page 7 8
Guidelines on drug use for children with diarrhoea
|
When to use drugs ANTlBlOTlCS should only be used for:
- dysentery (bloody diarrhoea - see="su55.htm">centre supplement), or
- suspected cholera when there is severe dehydration.
Otherwise, they are ineffective and should not be given, ANTI-PARASITIC drugs should only be used for:
- amoebiasis, if (in the case of bloody diarrhoea) antibiotic treatment for Shigella
has failed, or trophozoites of E. histolytica (the active
amoeba form) containing red blood cells are seen in the faeces
- giardiasis, when diarrhoea has lasted 14 days or more and
cysts or trophozoites of Giardia are seen in the faeces or small bowel fluid.
|
Key drugs to avoid ANTI-DIARRHOEAL drugs and ANTI-EMETICS should never be used. None has
proven practical value. Some are dangerous. The following drugs, commonly misused to treat diarrhoea, should not be given
to children with diarrhoea:
- Loperamide
Generic name: loperamide hydrochloride
Some brand names: Imodium, Arret, Imosec, Loperium, Vacontil, Lopemid
- Diphenoxylate
Generic name: diphenoxylate hydrochloride with atropine sulphate
Some brand names: Lomotil, Reasec, Lyspafen
- Hydroxyquinolines
Drugs containing: clioquinol (iodochlorhydroxyquin), iodoquinol (di-iodohydroxyquin), or
broxyquinoline
Some brand names: Entero-Vioform, Mexaform
- Non-absorbable sulphonamides
Examples: sulphaguanidine and sulphaphthalazole
- Adsorbents
Examples: kaolin, pectin, attapulgite and smectite
- Anti-diarrhoeals containing antibiotics
Examples: mixtures containing neomycin or streptomycin
For more information about drug use for diarrhoea see DDs="dd42.htm">42,
43 and 44, and the Drugs and Diarrhoea
supplement in DD50. |
Regulatory actions against anti-diarrhoeals taken around the world in 1990-92
| COUNTRY |
DRUGS AFFECTED |
ACTION |
DATE |
| France |
Brand-name paediatric product
containing loperamide |
Restriction on use in children |
August 1991 |
| India |
Fixed-dose combinations of
kaolin-pectin with absorbable drugs |
Sale and manufacture banned |
February 1991 |
| Indonesia |
Paediatric formulations of
loperamide
94 brand-name anti-diarrhoeal products containing antibiotic mixtures, hydroxyquinolines,
non-absorbable sulphonamides, and other substances |
Banned
Deregistration of solid and liquid formulations |
November 1990
October 1991 |
| Lebanon |
All products containing
loperamide, diphenoxylate, diphenoxine and ~ furazolidone
All liquid forms of streptomycin |
Restriction on use in children,
deregistration and banning of products |
August 1991 |
Libyan
Arab
Jamahiriva |
10 brand-name
anti-diarrhoeal products, which include substances such as anti-motility drugs,
anti-microbials, and adsotients |
Use in children banned |
May 1990 |
| Mexico |
5 brand-name paediatric products,
containing loperamide and diphenoxylate |
Deregistered |
December 1990 |
| Nepal |
Liquid preparations of
diphenoxylate and loperamide
Several combination drugs used as anti-diarrhoeals |
lmport and export banned
Production and sale banned |
August 1991
February 1992 |
| Pakistan |
3 brand-name combination drugs
used as anti-diarrhoeals
Drop and syrup forms of loperamide, diphenoxylate and pipenzolate |
Deregistered
Banned and withdrawn from market |
1989-90
June 1990 |
| Peru |
Paediatric formulations of
loperamide |
Deregistered |
October 1990 |
| Philippines |
Loperamide and diphenoxylate |
Deregistered |
September 1991 |
Republic
of Korea |
Loperamide |
Restriction on use in children |
May 1991 |
| Sri Lanka |
Syrup formulations of loperamide |
Desregistered |
November 1990 |
| Thailand |
Liquid preparations of
diphenoxylate
Liquid preparations of loperamide |
Desregistered
Desregistered |
February 1992
March 1992 |
| Turkey |
Drop and syrup formulations
containing loperamide |
Banned |
September 1991 |
|
DDOnline Dialogue
on Diarrhoea Online Issue no. 55 December
1993-February 1994  7 Page 8 7 Page 8
Prescribing habits changed As a result of reading DD over the past 12 years I have really changed my
prescribing habits. I have learnt that about 90 per cent of my patients do not need
antibiotics. Most diarrhoea is self-limiting. All that most patients require is the
replacement of lost fluids and electrolytes. Michael Chilembo, Clinical Officer, Tazara Residential Clinic,
Mpika, Zambia.
Are laboratory tests needed? As a registered nurse, I am very aware that the first line of treatment for diarrhoea
is rehydration. However, DD does not explain whether there is any need to find out
the cause of diarrhoea through laboratory analysis of a stool sample. If the diarrhoea is a result of bacteria, then giving oral rehydration alone is not
enough. It would be like leaving a water tap on, while trying to sweep up the water. The
tap has to be turned off. Shuka Balewa Tsams, General Hospital, Kaltungo, Bauchi State, Nigeria.
Dr Nathaniel Pierce, CDD, WHO replies: It is tempting to think that diarrhoea is caused by infection, therefore it should be
treated with an antibiotic. But several studies have shown that the routine use of
antibiotics for treating diarrhoea has no benefit, and may cause serious side effects. Why are antibiotics ineffective? First, many episodes of diarrhoea are caused by
viruses or protozoa (or even some bacteria) for which no antibiotic is effective. Second,
even when a bacteria treatable by an antibiotic is the cause, it is usually not possible
to determine which antibiotic should be used. Very few laboratories in the world can
identify all types of bacteria that cause diarrhoea, and even these take several days to
give an answer. There are two situations, however, where antibiotics are effective and should be given.
The first is children with bloody diarrhoea (see="su55.htm">centre supplement).
The second is anyone with suspected cholera and severe dehydration. In both cases, an
antibiotic can help to shorten the illness.
Better business in drugs
Parents complain that ORS is not a medicine to stop diarrhoea. If a doctor gives ORS
only, then parents change to a doctor who will prescribe drugs. Doctors who recommend
drugs are getting more business. What can be done to stop this? Dr M D Sayedul Haq, PO Box 306, Bojnord, Khorasan, Iran.
Dr Pierce replies: Doctors should help parents understand what to expect.during an illness, and how
treatment will help. For acute diarrhoea, they should explain that the illness will soon
stop by itself and that drugs cannot make it stop any earlier; that they are a waste of
money and may have dangerous side effects. It should be explained that ORS solution will
help the child to feel stronger and eat better even before the diarrhoea stops. Doctors
should ask the parents to bring the child back if he or she shows danger signs (poor
eating or drinking, passing of many watery stools, severe thirst, frequent vomiting,
fever, blood in the stools, no improvement), and make it clear that they would be happy to
see the child again if the parents are worried. It should also be mentioned that doctors have an obligation to treat patients
correctly, regardless of what patients may demand or other doctors practise.
Drug peddling in Nigeria Antibiotic abuse is a serious problem here. Imagine drug sellers with little education,
let alone medical knowledge, peddling antibiotics in the street, just like any other
market commodity. Such people are allowed to perform the role of doctor, pharmacist,
laboratory scientist and nurse. These peddlers rarely sell more than a single dose at a time, promising it will work
miracles. Storage conditions are far from ideal with sensitive drugs being subjected to
harsh sunlight and high temperatures. Amizan Mohammed Barau, Pharmacist, Murtala Mohammed Specialist Hospital,
Kano,
Nigeria.
Mr Robert Hogan, CDD, WHO replies: Mr Barau is right to be concerned about the selling of drugs by unlicensed and
untrained drug peddlers. This practice is extremely dangerous and local authorities should
take steps to stop such practices. Professional associations, such as pharmacists'
organisations, may encourage such actions. The public also needs to be informed of the danger of taking drugs without a doctor's
advice; the risks of taking the wrong drug or drugs of dubious quality; and the importance
of taking the correct dose for the right number of days.
NGO nutrition strategies DD53 incorrectly stated that an NGO working group was set
up by the International Conference on Nutrition (ICN) in 1992. The group referred to in DD
involved NGOs with representatives in Switzerland. On the other hand, a large
percentage of NGOs attending the conference belonged to the ICN NGO Consortium, an
international grouping which was responsible for valuable NGO contributions to the
Declaration and Plan of Action. Nancy Jo Peck, IBFAN representative to the ICN, C/o GIFA, PO Box 157, CH-1211 Geneva
19, Switzerland.
|

Scientific editors Dr Katherine Elliott and Dr William Cutting
Executive editor Kate O'Malley
Managing editor Kathy Attawell
Design & production Ingrid Emsden
Editorial advisory group
Professor A G Billoo (Pakistan)
Professor David Candy (UK)
Dr Shanti Ghosh (India)
Dr Michael Gracey (Australia)
Dr Nicole Guérin (France)
Dr Norbert Hirschhorn (USA)
Dr Sharon Huttly (UK)
Dr Claudio Lanata (Peru)
Dr Jon Rohde (USA)
Dr Mike Rowland (UK)
Professor Dang Duc Trach (Vietnam)
Professor Andrew Tomkins (UK) With support from AID (USA), Charity Projects (UK),
Ministry of
Development Cooperation (Netherlands), ODA (UK), UNICEF, WHO Publishing partners
BRAC (Bangladesh)
CMAI (India)
CMU (China)
Grupo CID (USA)
lmajics (Pakistan)
ORANA (Senegal)
RUHSA (India)
Turkish Medical Association (Turkey)
Consultants at University Eduardo Mondlane (Mozambique)
|
Issue no. 55 December 1993 - February 1994
Page Navigation
This edition of Dialogue on Diarrhoea Online is produced by Rehydration Project. Dialogue on Diarrhoea was published four times a year in English, Chinese, French, Portuguese, Spanish, Tamil,
English/Urdu and Vietnamese and reached more than a quarter of a million readers worldwide. The English edition of Dialogue on Diarrhoea was produced and distributed by Healthlink Worldwide. Healthlink Worldwide is committed to strengthening primary health care and
community-based rehabilitation in the South by maximising the use and impact
of information, providing training and resources, and actively supporting
the capacity building of partner organisations. - ISSN 0950-0235 Reproducing articles
Healthlink Worldwide encourages the reproduction of
articles in this newsletter for non-profit making and educational uses. Please
clearly credit Healthlink Worldwide as the source and, if possible, send us a copy of any uses made of the material.
|
updated: 23 April, 2014
updated: 23 April, 2014
|